Deputy Study Director
Priv.-Doz. Dr. med. habil. Benjamin Friedrichson, MHBA
Dr. Benjamin Friedrichson is a distinguished anaesthesiologist and clinical scientist. He studied medicine at Goethe University in Frankfurt and furthered his expertise by earning a Master of Health Business Administration from FAU Erlangen-Nürnberg. His academic background and advanced training uniquely position him at the intersection of clinical practice and healthcare management, allowing him to contribute significantly to both fields. Dr. Friedrichson's work is characterized by a commitment to integrating clinical excellence with innovative healthcare business practices.
15 Years
Recent Publications
Perfusion. 2026.
Artificial intelligence-guided tools in adult ECMO: Current advancements, emerging Trends and future directions.
IntroductionExtracorporeal membrane oxygenation (ECMO) provides life support for patients with refractory cardiac or respiratory failure. The complexity of ECMO management and associated mortality necessitates high-accuracy clinical decision-making systems. Artificial intelligence (AI) has emerged as a potential approach to address challenges in ECMO management, from patient selection to real-time assessment and outcome prediction.ObjectiveTo synthesize the current evidence of AI application in adult ECMO, addressing predictive modelling for patient outcomes, real-time decision support systems, and complication prevention, as well as the evolving regulatory challenges governing medical AI deployment in critical care settings.MethodsA narrative literature review was conducted across PubMed/MEDLINE, Embase, Cochrane Library, IEEE Xplore, and preprint servers (arXiv/medRxiv). The search strategy combined ECMO-relevant terms ("V-A ECMO", "V-V ECMO") with AI terminologies ("artificial intelligence", "machine learning", "deep learning", "digital twin"). Studies were included if they focused on adult cohorts (age ≥18 years) and were published in English between 2018 and 2025.ResultsThe review found several AI algorithms under development for different stages of ECMO therapy. AI algorithms have been developed to assist in the initiation, prognostication, complication detection, real-time control, and weaning of ECMO. However, none have been clinically translated thus far.ConclusionWhile AI for precision ECMO management is promising, several prerequisites remain unmet, including the integration of high-frequency device data, prospective external multicenter validation, and the development of robust regulatory frameworks. Securing these advances will bridge the gap between algorithm development and the clinical arena.
Int J Emerg Med. 2026.
Time to intubate with an innovative intubation device: a dual-center randomized crossover non-inferiority simulation study.
Endotracheal intubation is a high-stakes intervention in emergency airway management, with patient safety closely linked to first-pass success and avoidance of repeated attempts. The Frankfurt Intubation Device (FID) is a bougie-inspired intubation device intended to provide fast protection against aspiration once positioned in the trachea.
J Cardiovasc Dev Dis. 2026.
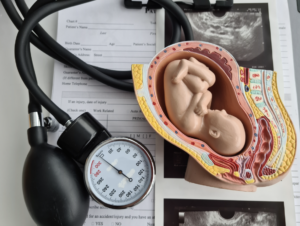
Clinical Characteristics and Outcomes of 1894 Women with Peripartum Cardiomyopathy Treated with and Without Levosimendan in Germany.
Peripartum cardiomyopathy (PPCM) is a rare form of heart failure occurring during the last month of pregnancy or within five months postpartum. While levosimendan is considered beneficial in heart failure and cardiogenic shock, evidence supporting its use in PPCM is limited. This study investigated the prevalence of PPCM in Germany and evaluated outcomes associated with levosimendan use.
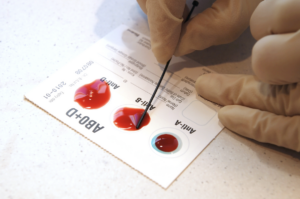
Blood Transfus. 2026.
Transfusion practice in elderly patients across surgical disciplines in Germany - a secondary data analysis of over 21 million patients.
Clinicians are increasingly confronted with elderly patients across nearly all surgical disciplines. Advanced age is an independent risk factor for complications, prolonged hospitalization, and particularly for red blood cell (RBC) transfusion. The elderly suffer more frequently from anemia, which is associated with higher perioperative transfusion requirements, increased complication rates, and mortality Surgical disciplines differ not only in primary diagnoses but also in the demographics of their typical patient population.
J Cardiothorac Vasc Anesth. 2026.
Preservation of Platelet Function After Intraoperative Cell Salvage Using the i-SEP Same Device in Cardiac Surgery.
To evaluate whether platelet function is preserved after intraoperative autotransfusion using the Same system, a device designed to retain both red blood cells and platelets in patients undergoing on-pump cardiac surgery.
Eur J Trauma Emerg Surg. 2025.
Frequency and patterns of CMF emergency cases during and after COVID-19.
Craniomaxillofacial (CMF) trauma constitutes a significant proportion of hospital presentations, often resulting from high-energy mechanisms such as interpersonal violence and traffic accidents. The COVID-19 pandemic and associated public health restrictions markedly altered daily life and social behavior, potentially influencing trauma patterns and emergency healthcare utilization.
Sci Rep. 2025.
Critical risks of haemoadsorption for COVID-19 patients and directions for future evaluations: a nationwide propensity score matched cohort study.
Haemoadsorption has been suggested as treatment adjunct for sepsis and septic shock, cardiac surgery, acute respiratory distress syndrome, and coronavirus disease 2019 (COVID-19). Randomised clinical trials did not provide conclusive evidence for benefits and even suggest risks in COVID-19 patients. Retrospective observational cohort study based on hospital remuneration data from all COVID-19 patients treated in intensive care units in Germany between 01/01/2020 and 12/31/2021. Regression modelling was performed for 1:1 propensity score matching of 2058 patients. Two-sided probability values for group comparisons and regression models with spline functions controlling for non-linear relationships and medically relevant interaction variables were calculated. In-hospital mortality of patients supported with haemoadsorption was significantly higher compared to matched control patients (74.6% vs. 70.3%, p = 0.0299). Haemoadsorption was associated with coagulopathy (68.0% vs. 54.9%, p < 0.0001), cardiac arrhythmia (49.2% vs. 44.2%, p = 0.0272), and cardiopulmonary resuscitation (CPR, 19.3% vs. 13.1%, p = 0.0002). Further, haemoadsorption increased the chance of death for COVID-19 patients without septic shock (odds ratio, OR [within a 95% confidence interval, CI]; 1.40 [1.05-1.86]) and did not improve survival of septic shock patients (1.19 [0.85-1.67]). Independent variables with a significant impact on mortality included the use of extracorporeal membrane oxygenation (ECMO, 2.15 [1.68-2.76]) and CPR (1.60 [1.03-2.45]). The timing of the haemoadsorption therapy had no effect on patients´ outcomes. Due to inconclusive evidence for benefit and potential harm, haemoadsorption therapy should be limited to thoroughly designed clinical trials before introduced into clinical routine in the context of COVID-19.
Sci Rep. 2024.
Extracorporeal membrane oxygenation in cardiovascular medication poisoning. A German-wide retrospective study.
Medication poisoning, resulting from the ingestion of cardiotoxic drugs, presents a significant health issue. The mortality rate remains high for patients with myocardial dysfunction refractory to conventional treatments. Venoarterial Extracorporeal Membrane Oxygenation (V-A ECMO) provides temporary support, potentially enhancing patient outcomes. This study aims to assess the efficacy of V-A ECMO in treating cardiovascular failure induced by cardiovascular medication poisoning. We utilized inpatient data from all hospitalisations in Germany from 2007 to 2022 due to cardiovascular medication poisoning treated with V-A ECMO. Patient characteristics, comorbidities, complications and application of ECMO were described descriptively and analysed for statistical significance between survivors and non-survivors. Overall, 49 patients received V-A ECMO for cardiovascular medication poisoning, with a survival rate of 63.6%. The most ingested medications were calcium-channel blockers (38.8%) and beta-adrenoceptor antagonists (34.7%). Half of non-survivors received in-hospital CPR, compared to 12.9% of survivors. Early ECMO implantation (within 24 h of admission) was common (83.7%) but did not significantly impact survival rates. A substantial number of patients presented with multiple substances ingested. V-A ECMO represents a viable option for patients experiencing cardiac failure due to medication poisoning. A structured implementation of V-A ECMO for cardiovascular medication poisoning could lead to higher survival rates.
J Crit Care. 2024.
The value of artificial intelligence for the treatment of mechanically ventilated intensive care unit patients: An early health technology assessment.
The health and economic consequences of artificial intelligence (AI) systems for mechanically ventilated intensive care unit patients often remain unstudied. Early health technology assessments (HTA) can examine the potential impact of AI systems by using available data and simulations. Therefore, we developed a generic health-economic model suitable for early HTA of AI systems for mechanically ventilated patients.
J Clin Med. 2024.
Polyuria in COVID-19 Patients Undergoing Extracorporeal Membrane Oxygenation.
: The COVID-19 pandemic caused an unprecedented number of patients requiring veno-venous extracorporeal membrane oxygenation (VV ECMO) therapy. Clinical polyuria was observed at our ECMO center during the pandemic. This study aims to investigate the incidence, potential causes, and implications of polyuria in COVID-19 patients undergoing VV ECMO therapy. : Here, 68 SARS-CoV-2 positive patients receiving VV ECMO were stratified into the following two groups: polyuria (PU), characterized by an average urine output of ≥3000 mL/day within seven days following initiation, and non-polyuria (NPU), defined by <3000 mL/day. Polyuria in ECMO patients occurred in 51.5% (n = 35) within seven days after ECMO initiation. No significant difference in mortality was observed between PU and NPU groups (60.0% vs. 60.6%). Differences were found in the fluid intake ( < 0.01) and balance within 24 h ( = 0.01), creatinine ( < 0.01), plasma osmolality ( = < 0.01), lactate ( < 0.01), urea ( < 0.01), and sodium levels ( < 0.01) between the groups. Plasma osmolality increased ( < 0.01) after ECMO initiation during the observation period. : Diuresis and plasma osmolality increased during VV ECMO treatment, while mortality was not affected by polyuria. : Polyuria does not appear to impact mortality. Further investigations are warranted to elucidate its underlying mechanisms and clinical implications in the context of VV ECMO therapy and COVID-19 management.
Br J Anaesth. 2024.
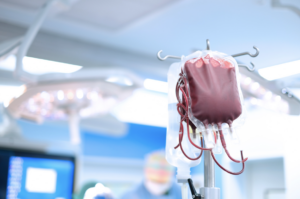
Use of cell salvage in obstetrics in Germany: analysis of national database of 305 610 cases with peripartum haemorrhage.
One of the leading causes of maternal death worldwide is severe obstetric haemorrhage after childbirth. Use of intraoperative cell salvage is strongly recommended by international guidelines on patient blood management. Recent data provide strong evidence that use of cell salvage in obstetrics is effective and safe in women with postpartum haemorrhage resulting in fewer transfusion-related adverse events and shorter hospital stay. We retrospectively analysed the use of cell salvage in bleeding women during delivery for a period of 10 yr in German hospitals.
Pharmacoeconomics. 2024.
Lessons Learned from Model-based Economic Evaluations of COVID-19 Drug Treatments Under Pandemic Circumstances: Results from a Systematic Review.
Following clinical research of potential coronavirus disease 2019 (COVID-19) treatments, numerous decision-analytic models have been developed. Due to pandemic circumstances, clinical evidence was limited and modelling choices were made under great uncertainty. This study aimed to analyse key methodological characteristics of model-based economic evaluations of COVID-19 drug treatments, and specifically focused on modelling choices which pertain to disease severity levels during hospitalisation, model structure, sources of effectiveness and quality of life and long-term sequelae.
J Med Syst. 2024.
Web-based Dashboard on ECMO Utilization in Germany: An Interactive Visualization, Analyses, and Prediction Based on Real-life Data.
In Germany, a comprehensive reimbursement policy for extracorporeal membrane oxygenation (ECMO) results in the highest per capita use worldwide, although benefits remain controversial. Public ECMO data is unstructured and poorly accessible to healthcare professionals, researchers, and policymakers. In addition, there are no uniform policies for ECMO allocation which confronts medical personnel with ethical considerations during health crises such as respiratory virus outbreaks.Retrospective information on adult and pediatric ECMO support performed in German hospitals was extracted from publicly available reimbursement data and hospital quality reports and processed to create the web-based ECMO Dashboard built on Open-Source software. Patient-level and hospital-level data were merged resulting in a solid base for ECMO use analysis and ECMO demand forecasting with high spatial granularity at the level of 413 county and city districts in Germany.The ECMO Dashboard ( https://www.ecmo-dash.de/ ), an innovative visual platform, presents the retrospective utilization patterns of ECMO support in Germany. It features interactive maps, comprehensive charts, and tables, providing insights at the hospital, district, and national levels. This tool also highlights the high prevalence of ECMO support in Germany and emphasizes districts with ECMO surplus - where patients from other regions are treated, or deficit - origins from which ECMO patients are transferred to other regions. The dashboard will evolve iteratively to provide stakeholders with vital information for informed and transparent resource allocation and decision-making.Accessible public routine data could support evidence-informed, forward-looking resource management policies, which are urgently needed to increase the quality and prepare the critical care infrastructure for future pandemics.
Front Med (Lausanne). 2024.
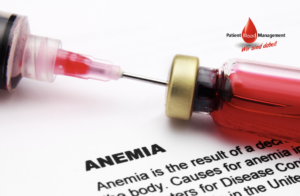
Maternal anemia and red blood cell requirements in 72 women undergoing intrapartum treatment (EXIT) procedure.
The intrapartum treatment (EXIT) allows to ensure fetal airway while keeping uteroplacental circulation. However, EXIT may become a life-threatening procedure due to the increased risk of uterine atony or placenta abruption with increased peripartum blood losses and increased transfusion rates. We aim to review maternal anemia prevalence and transfusion requirements in women undergoing EXIT procedure.
Antibiotics (Basel). 2024.
No Sequestration of Commonly Used Anti-Infectives in the Extracorporeal Membrane Oxygenation (ECMO) Circuit-An Ex Vivo Study.
Patients undergoing extracorporeal membrane oxygenation (ECMO) often require therapy with anti-infective drugs. The pharmacokinetics of these drugs may be altered during ECMO treatment due to pathophysiological changes in the drug metabolism of the critically ill and/or the ECMO therapy itself. This study investigates the latter aspect for commonly used anti-infective drugs in an ex vivo setting. A fully functional ECMO device circulated an albumin-electrolyte solution through the ECMO tubes and oxygenator. The antibiotic agents cefazolin, cefuroxim, cefepime, cefiderocol, linezolid and daptomycin and the antifungal agent anidulafungin were added. Blood samples were taken over a period of four hours and drug concentrations were measured via high-pressure liquid chromatography (HPLC) with UV detection. Subsequently, the study analyzed the time course of anti-infective concentrations. The results showed no significant changes in the concentration of any tested anti-infectives throughout the study period. This ex vivo study demonstrates that the ECMO device itself has no impact on the concentration of commonly used anti-infectives. These findings suggest that ECMO therapy does not contribute to alterations in the concentrations of anti-infective medications in severely ill patients.
Registry Study for Research of Blood Donor and Recipient Long-Term Outcomes
The latest news, articles, and resources on transfusion medicine – follow our deputy study director, Dr Jan Kloka, on LinkedIn.
Address
Universitätsklinikum
Frankfurt am Main
KAIS – Haus 13a
Theodor-Stern-Kai 7
60596 Frankfurt am Main
Contact
© Copyright 2024 by transfusionregistry.org